Have you ever felt a pain so sharp, so sudden, that it stole your breath before you could understand what was happening? Some describe it as a burning deep in the gut, others say it feels like a tight fist squeezing them from the inside. If you’ve ever heard of pancreatitis, you may know that people call it “the pain you can’t survive” for a reason. But what most don’t realize is that behind this frightening phrase lies a story of warning signs, hidden causes, and quiet opportunities to protect your health before things get worse.
Stay with me, because what you’ll learn today might help you recognize symptoms sooner, understand your risks, and take steps that empower—not frighten—you. And the most eye-opening part? That comes near the end.
Why Pancreatitis Deserves More Attention Than Most People Give It
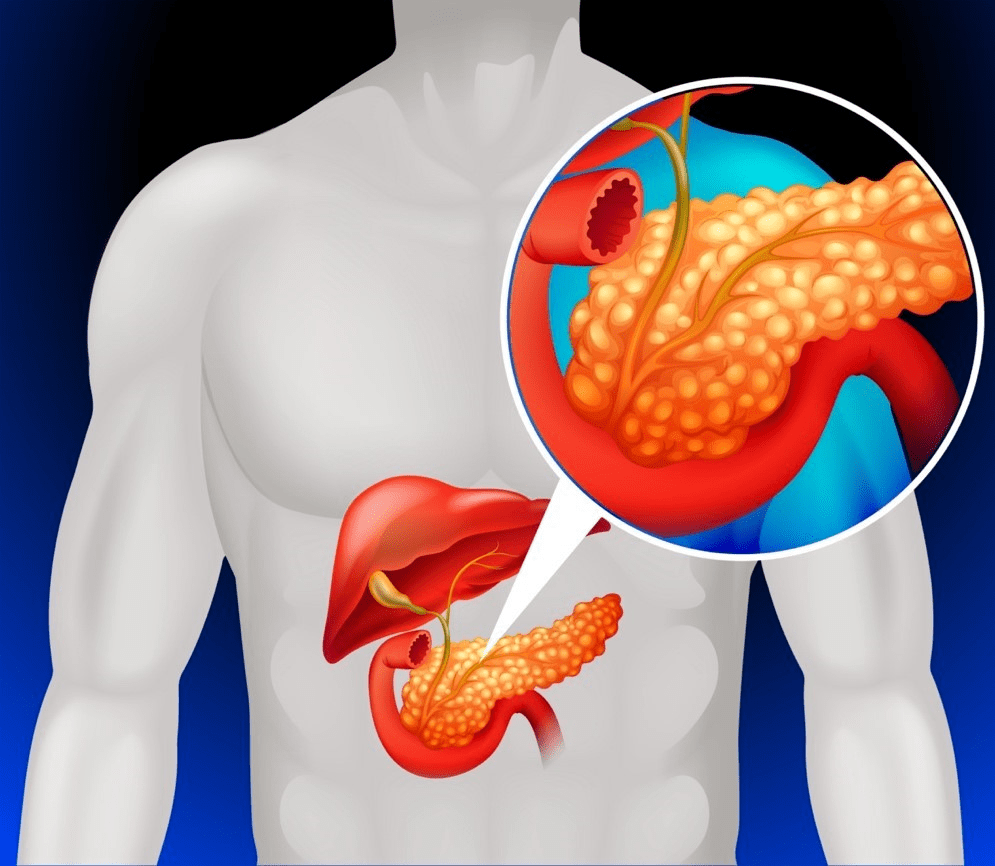
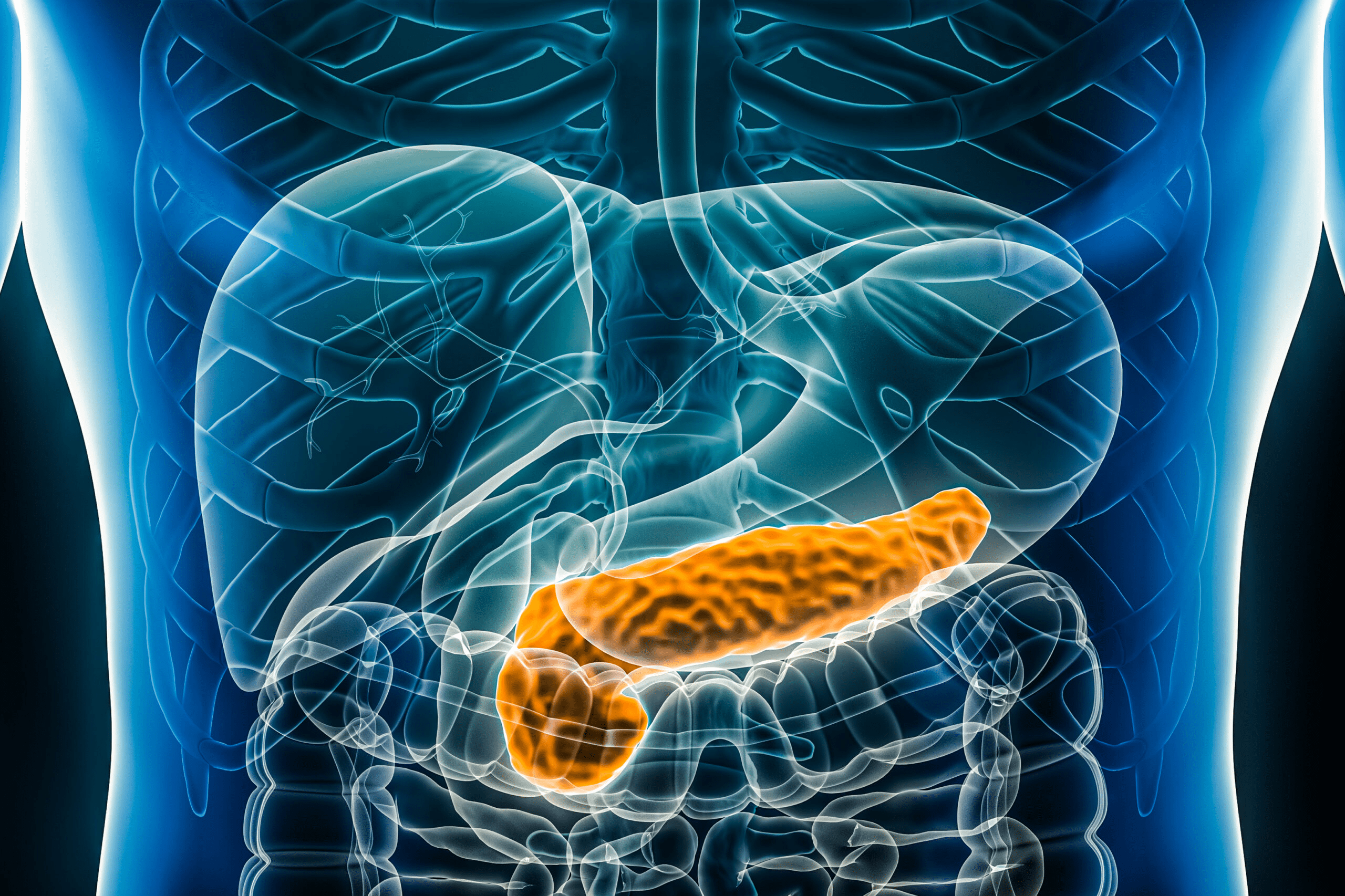
Pancreatitis isn’t just stomach pain. It’s inflammation of an organ that quietly supports digestion, metabolism, and even blood sugar balance. When the pancreas becomes inflamed, the digestive enzymes it normally releases can turn inward and irritate the organ itself.
The pain can be overwhelming. Many describe it as pain radiating to the back, making it impossible to stand straight, breathe comfortably, or find relief. And the most alarming part? Many people ignore early signs because they seem like “ordinary stomach problems.”
That leads us to the question more people should be asking:
What actually triggers pancreatitis—and could you be overlooking something important?
The Countdown: 7 Hidden Factors That Could Increase Your Risk
Each of the following insights begins with a real-life scenario—not medical advice, but relatable stories based on common patterns people report. And each one ends with a subtle clue, pulling you into the next piece of the puzzle.
7. The “weekend habits” that stay in your system longer than you think
Mark, 54, loved weekend barbecues. A couple of beers, maybe a cocktail… nothing “excessive.” But over time, alcohol could irritate the pancreas, making it more vulnerable. He brushed off the mild upper abdominal discomfort until one day the pain became unbearable.
People often underestimate how repeated small exposures can add up.
And that brings us to a factor many ignore entirely.

6. Gallbladder issues that quietly affect the pancreas
Susan, 61, noticed on-and-off pain under her right rib cage. She assumed it was acid reflux. Weeks later, a gallstone blocked her bile duct and triggered pancreatitis.
Gallstones are one of the most common underlying causes, but because symptoms can be mild at first, many don’t connect the dots.
This leads us to something even less discussed.
5. The role of medications you don’t think twice about
Some medications—certain antibiotics, diuretics, or immune-modulating drugs—could irritate the pancreas in rare cases. James, 67, only realized this after reading the tiny print on a bottle he’d taken for years.
He had dismissed earlier digestive pain as “aging.”
But aging alone isn’t the only hidden factor…
4. High triglycerides that build up silently
Imagine Lisa, 59, who enjoyed homemade desserts. She felt fine—until routine bloodwork showed extremely high triglycerides. Levels above a certain threshold may increase pancreatitis risk, yet many people never test for it until symptoms appear.
If this sounds concerning, wait until you learn what happens next.
3. An overlooked connection: dehydration and enzyme imbalance
Few people associate dehydration with pancreatic stress. But the pancreas depends on proper fluid balance. Tom, 63, who rarely drank water, experienced severe cramping long before he realized how dehydration could affect digestion.
And this leads us to an even deeper layer…
2. Chronic inflammation from everyday habits
Stress, irregular eating, smoking, and high-fat meals can all contribute to low-grade inflammation. Over time, the pancreas can become more sensitive. Paula, 65, never imagined her rushed lifestyle might play a role in her digestive discomfort.
And now—the most important clue of all.
1. Ignoring early warning signs because they “seem normal”
Most people overlook the earliest signs:
A dull ache after eating.
Nausea that comes and goes.
Pain that feels like “a tight belt” around the upper stomach.
Back pain with no clear reason.
These often appear days or weeks before a serious episode.
Recognizing them early truly makes a difference.
Now that you know the hidden factors, let’s break down how pancreatitis affects the body in practical terms.
Understanding the Pancreas: A Simple Breakdown
| Function | What the Pancreas Does | What Happens When It’s Inflamed |
|---|---|---|
| Digestion | Produces enzymes to break down fats, proteins, carbs | Enzymes may activate too early, causing irritation |
| Blood Sugar | Releases insulin and glucagon | Balance may become unpredictable |
| Hormonal Regulation | Supports metabolic signals | Body may struggle with appetite or energy |
| Protection | Manages inflammation responses | Inflammation can spread or intensify |
Understanding this helps you see why pancreatitis feels so intense—and why paying attention matters.
“But what can I do?” — The Part Everyone Wants to Know
Before we explore supportive steps, here’s a quick story.
Evelyn, 62, had mild abdominal pain for months. She assumed it was bloating, ignored it, and kept working long hours. When she finally saw a doctor, she learned her pancreas had been under significant stress.
Her turning point came when she said:
“I realized I was waiting for pain to get unbearable before taking it seriously.”
Her story is not rare—and that’s why supportive habits matter.
7 Supportive Habits That Could Help Protect Your Pancreatic Health
These are not cures or treatments. They’re simple habits people use to support digestive and pancreatic well-being. And the final one might change how you listen to your body.
7. Lighten your meals, especially at night
Heavier meals require more digestive effort. Many people report less discomfort when they choose lighter dinners with lean proteins and vegetables.
This sets the stage for the next habit.
6. Stay hydrated consistently
Water helps maintain enzyme flow. Not drinking enough could make digestion more difficult. Some people keep a bottle nearby to remind themselves.
Small changes often lead to bigger improvements.
5. Reduce alcohol intake when possible
Even small, regular amounts can strain the pancreas. Some people replace alcohol with herbal teas or sparkling water.
And something unexpected happens next…
4. Add healthy fats instead of heavy ones
Olive oil, avocado, and nuts may be easier on digestion than fried foods. People often report feeling “lighter” after meals when making this swap.
But here’s the surprising part.
3. Keep stress in check with tiny daily pauses
Stress doesn’t just affect the mind—it can influence digestion. A 5-minute breathing break could make a noticeable difference over time.
And what comes next is even more important.
2. Monitor your bloodwork regularly
Many underlying risks—like triglycerides or gallbladder concerns—don’t show symptoms at first. Routine checkups help you stay ahead, not behind.
Now for the most life-changing habit.
1. Pay attention to early signals from your body
No one knows your body better than you. If something feels “off,” don’t ignore it. Small signs often appear long before major symptoms.
This habit alone has changed countless lives.
How to Practice Pancreas-Friendly Habits Safely
| Habit | Safe Approach | Why It Helps |
|---|---|---|
| Hydration | Sipping water through the day | Supports digestive rhythms |
| Food choices | Lean meals, fewer fried items | Less strain on digestion |
| Stress breaks | Breathing, stretching, short rests | Reduces inflammation triggers |
| Monitoring | Routine medical checkups | Early awareness |
| Alcohol awareness | Reducing frequency | Supports long-term health |
“Maybe you’re wondering…” — Addressing Doubts People Commonly Have
Maybe you’re wondering: “Is pancreatitis always severe?”
Not always—some cases are mild, but symptoms can escalate quickly.
Maybe you’re thinking: “Could I really mistake it for something else?”
Yes, because early signs mimic indigestion, gallbladder issues, or back pain.
Maybe you’re asking: “Is there anything I can do today?”
There is: awareness, supportive habits, and paying attention to symptoms.
And now, let’s bring everything together.
The Solution: Awareness, Action, and Attentiveness
The truth about pancreatitis isn’t meant to scare you—it’s meant to empower you. Understanding your body, recognizing subtle signs, and building habits that support long-term health can make a real difference.
People like Mark, Susan, and Evelyn found their turning point not in fear, but in awareness.
You can too.
Conclusion: The Message You Should Not Ignore
If there’s one thing to take away today, it’s this:
Pancreatitis doesn’t usually appear out of nowhere. It sends whispers before it screams.
Listening early may help you avoid bigger problems later.
So here’s your action step:
Pay attention to how your upper abdomen feels after meals.
Notice patterns.
Keep your hydration steady.
Make small swaps and watch how your body responds.
And if something doesn’t feel right, speak up—your health is worth the conversation.
P.S. A surprising fact: the pancreas is only about six inches long, yet its influence on your body is enormous. Its quiet work is easy to overlook… until it needs your attention.
This article is for informational purposes only and does not replace professional medical advice. Consult a healthcare provider for personal guidance.