Have you noticed persistent foam in the toilet after urinating, like a layer of bubbles that lingers? For many over 45, this subtle change sparks quiet worry—especially when mornings bring the same sight day after day. You flush and wonder if it’s just dehydration or something more serious brewing inside.
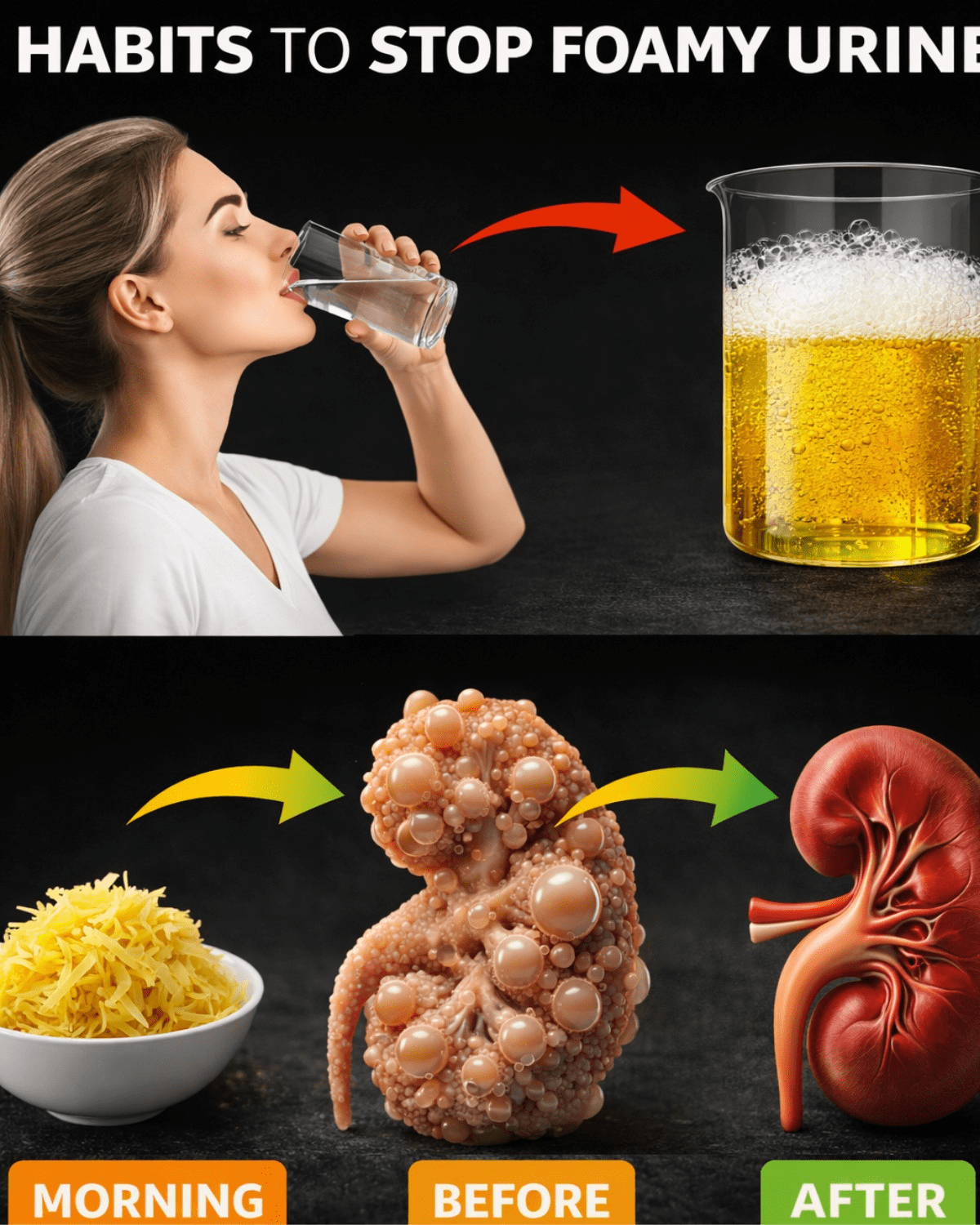
Foamy urine often stems from temporary factors like forceful urination or concentrated pee. Yet when it becomes consistent, it frequently points to excess protein leaking into the urine, a condition known as proteinuria. Proteinuria can signal underlying issues affecting kidney filtration, such as high blood pressure, diabetes, or early chronic kidney changes.
The good news? Simple, evidence-based habits may help support better kidney function and potentially lessen this symptom over time. Research shows lifestyle adjustments can influence proteinuria levels and overall kidney wellness. Let’s explore six practical, science-supported steps you can consider.
But first, understand why this matters so much right now.
Why Foamy Urine Deserves Your Attention After 45
As we age, kidneys work harder to filter waste amid shifting hormones, possible blood pressure rises, and accumulated stress. Proteinuria doesn’t always cause pain, so foamy urine becomes an early whisper from the body. Studies link persistent proteinuria to faster kidney function decline if unaddressed.
Occasional bubbles from dehydration or speed vanish quickly. Persistent foam, however, often ties to protein in urine and warrants professional evaluation. You might think it’s harmless, but many regret waiting when simple checks reveal treatable causes.
Keep reading—the first habit could make a noticeable difference faster than you expect.

6 Evidence-Based Habits to Help Support Kidney Health and Potentially Reduce Foamy Urine
Habit 6: Stay Well-Hydrated Every Day
Dehydration concentrates urine, sometimes creating temporary foam. Adequate fluids help kidneys flush waste efficiently and dilute urine naturally. Research consistently shows proper hydration supports overall kidney function.
Picture starting your day with a tall glass of water—urine turns lighter yellow, and foam often lessens. Aim for 1.5–2 liters daily, adjusting for activity and climate. Feel the difference in energy and clearer output. But hydration alone isn’t everything—habit 5 targets a key driver.
Habit 5: Embrace Moderate, Regular Physical Activity
Sedentary habits contribute to weight gain, higher blood pressure, and strain on kidneys. Regular exercise helps control these factors and may improve kidney blood flow. Studies on lifestyle interventions show physical activity links to better kidney markers, including reduced proteinuria risk in some populations.
Think of a 30-minute walk most days—your heart pumps stronger, blood pressure steadies, and kidneys thank you. Start gentle if new to movement. Many notice steadier energy and fewer swelling issues. The next habit builds directly on this foundation.
Habit 4: Manage Blood Pressure Through Everyday Choices
High blood pressure damages kidney filters over time, increasing protein leakage. Lifestyle steps like lower salt intake, exercise, and stress reduction often lower readings effectively. Evidence from cohort studies shows healthier overall lifestyles associate with lower incident proteinuria odds.
You check your pressure at home and see numbers trending down after small tweaks. Less strain means healthier filtration. Confidence grows as foam potentially eases. But blood pressure control pairs powerfully with habit 3.

Habit 3: Shift Toward a Kidney-Friendly Eating Pattern
Diets high in processed foods and excess sodium stress kidneys. Emphasizing fruits, vegetables, whole grains, and leaner proteins supports balance. Research, including meta-analyses, indicates plant-based approaches and moderated animal protein may reduce proteinuria impact on renal hemodynamics.
Imagine meals rich in colorful produce—antioxidants protect cells, sodium stays low, and kidneys work lighter. Many report feeling less bloated and seeing urine changes. This sets the stage for even stronger support. Habit 2 focuses on a specific dietary tweak.
Habit 2: Moderate Protein Intake Wisely
Excess dietary protein can burden kidneys, especially with existing concerns. Guided reduction eases filtration load in some cases. Evidence from reviews and trials suggests low-protein or plant-focused diets help control proteinuria, particularly in non-diabetic kidney issues.
You swap some meat for beans or veggies—protein needs stay met, but kidneys breathe easier. Consult a professional for personalized levels. Results build gradually but feel empowering. One more habit often amplifies all the others.
Habit 1: Prioritize Blood Sugar Stability If Relevant
Elevated blood sugar over years damages kidney vessels, leading to protein leakage. Stable levels through diet, movement, and monitoring protect filtration. For those with diabetes or prediabetes, tight control links to slower kidney changes and less proteinuria.
You monitor carbs, choose whole foods, and watch levels steady—foam may decrease as kidneys face less stress. This foundational step ties everything together for long-term wellness.
These habits work synergistically. Consistency creates the biggest shifts. Now let’s make them practical.
How to Get Started Safely and Effectively
Begin with one or two changes—small wins build momentum. Track urine appearance, energy, and any swelling over weeks. Pair habits with regular check-ins.
Practical Tips for Success
| Habit | Easy Starting Step | Why It Helps |
|---|---|---|
| Hydration | Drink a glass upon waking | Dilutes urine, supports filtration |
| Exercise | Walk 20-30 minutes daily | Controls BP and weight |
| Blood Pressure | Limit salt to under 2,300 mg/day | Reduces kidney strain |
| Eating Pattern | Add more veggies to every meal | Provides protective nutrients |
| Protein Moderation | Choose plant sources half the time | Eases kidney workload |
| Blood Sugar | Opt for whole grains over refined | Prevents vascular damage |
Always personalize—work with your doctor or a dietitian. Monitor progress through urine tests if recommended.
Important Safety Notes and Realistic Expectations
These habits support general kidney health but do not treat or cure conditions. Foamy urine can stem from serious issues—persistent cases need medical evaluation. See a healthcare provider promptly if foam continues, especially with swelling, fatigue, changes in urination, or known risks like diabetes or hypertension.
Medications like ACE inhibitors or ARBs often play a key role when prescribed. Lifestyle supports but does not replace professional care.
The article you are reading is for informational purposes only and does not replace professional medical advice. Please consult your healthcare provider for personalized guidance.
Stories from Real People
Consider Tom, 52, who noticed foamy urine during routine checks. After doctor-guided changes—more water, less salt, daily walks—his follow-up tests showed improvement. He felt more in control.
Lisa, 48, with prediabetes, adopted plant-heavy meals and steady exercise. Foam lessened, energy rose, and her confidence returned.
These examples highlight how consistent habits can contribute positively.
Your Next Step Toward Better Kidney Support
You now know six practical, backed ways to nurture your kidneys. Pick one habit today—perhaps that extra glass of water or a shorter salt goal. In weeks, you may notice subtle positive shifts.
Share this with a loved one facing similar concerns. Small daily choices compound into meaningful protection.
One bonus insight: Quitting smoking, if applicable, dramatically supports kidney health too—studies show major risk reduction.
Your kidneys deserve this gentle care. Start today and feel the difference.






