Picture this: You wake up scratching at your skin again, convinced something is crawling just beneath the surface. Tiny, colorful threads seem to emerge from slow-healing sores that never quite close. The itching feels relentless, like insects moving under your flesh, and no matter how much you pick or wash, the sensation persists. For many who experience these symptoms, the distress is profound—yet medical explanations remain divided and uncertain. This is the challenging reality of Morgellons disease, a condition that has sparked intense debate since it gained attention in the early 2000s. While some describe it as a mysterious emerging illness, the broader medical community views it through a different lens. Let’s explore what is currently understood about this enigmatic disorder.

Morgellons disease (often abbreviated MD) refers to a set of symptoms where individuals report unusual fibers or filaments appearing in or emerging from the skin, accompanied by intense sensations and non-healing lesions. The term was coined in 2002 by Mary Leitao after observing similar symptoms in her child. Despite widespread patient reports, no universally accepted diagnostic criteria exist, and research findings often conflict.
The condition affects a small number of people, predominantly middle-aged Caucasian women, though cases appear across demographics. It can profoundly impact quality of life, with recent studies showing lower scores compared to conditions like psoriasis or atopic dermatitis. Have you ever felt dismissed when describing unexplained skin issues? For many with these experiences, that feeling is all too common.
How Morgellons Disease May Develop
The exact origin of Morgellons disease remains one of medicine’s unresolved questions. The most widely accepted view, supported by major health organizations, is that it represents a form of delusional infestation (also called delusional parasitosis), where individuals hold a fixed belief in skin infestation despite lack of evidence for parasites or external materials.
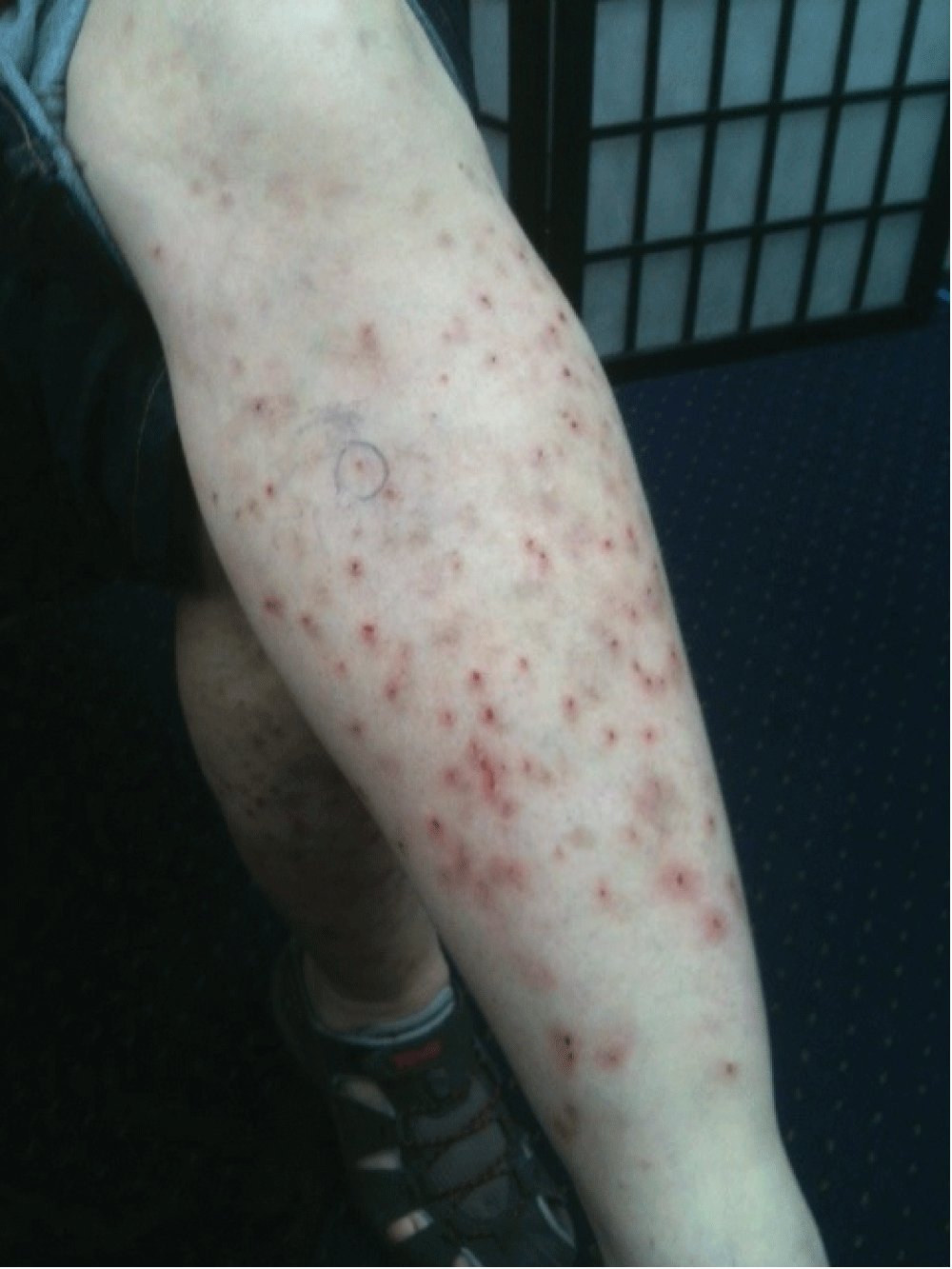
A landmark 2012 study by the Centers for Disease Control and Prevention (CDC) examined 115 individuals reporting these symptoms. Researchers found no evidence of infectious agents or parasites. The fibers examined were typically composed of cotton, skin fragments, or other environmental contaminants, likely introduced through repeated scratching and picking.
Some smaller studies and patient advocacy groups propose alternative explanations, including possible links to Borrelia burgdorferi (the bacterium associated with Lyme disease) or other spirochetal infections. These findings remain controversial and are not supported by larger, independent investigations. Environmental factors, chronic itching from other skin conditions, or underlying psychiatric factors may contribute in some cases. But what does it actually feel like for those affected?
Recognizing the Signs and Symptoms
The hallmark of Morgellons disease is the perception of fibers—often described as red, blue, black, white, or multicolored—embedded in, lying under, or protruding from the skin. Patients frequently collect these materials and present them to doctors (known as the “matchbox sign” or “specimen sign”).
Common symptoms include:
- Intense crawling, stinging, biting, or prickling sensations (formication)
- Persistent itching leading to compulsive scratching
- Slow-healing or non-healing skin sores, often self-inflicted erosions
- Burning pain in affected areas
- Fatigue, joint pain, sleep disturbances, or cognitive difficulties in some reports
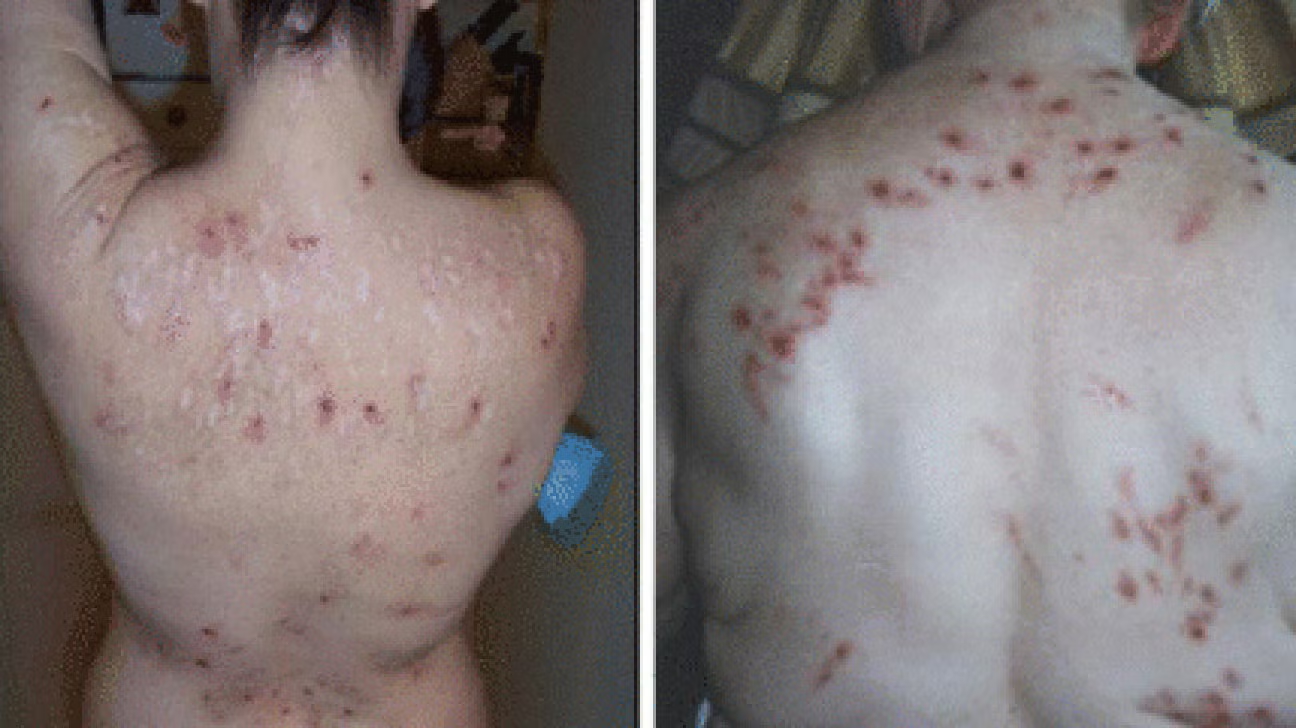
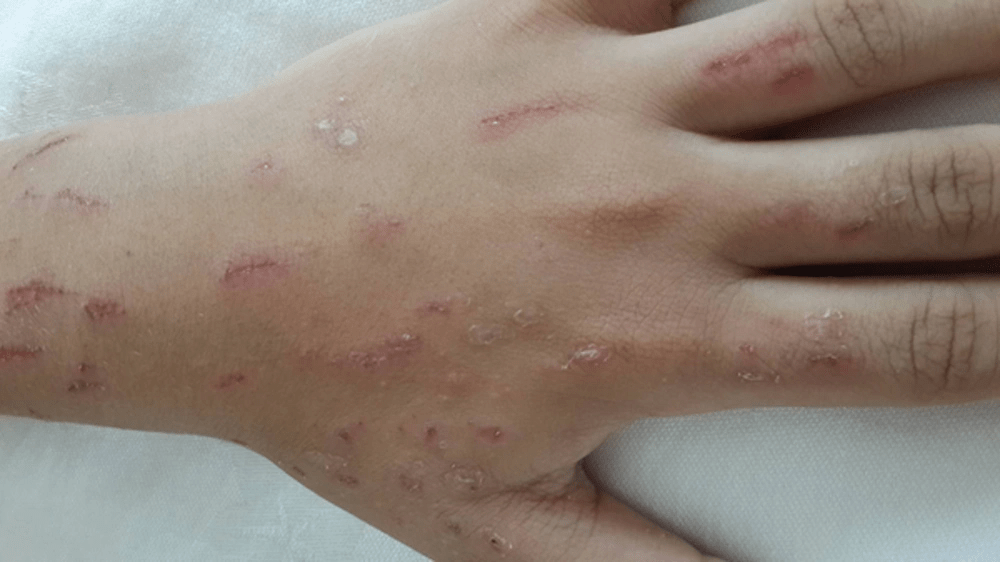
These symptoms can cause significant emotional distress, including anxiety, depression, and social isolation. Lesions typically appear in reachable areas like arms, hands, face, and legs, sparing hard-to-reach spots—a pattern often seen in conditions involving repetitive picking.
Here are examples of what patients frequently describe:
- A stinging sensation that feels like something is trying to “penetrate” from inside the skin
- Fibers that appear thread-like, wiry, or even floral-shaped under magnification
- Open sores that scab repeatedly but never fully resolve
But why do these fibers appear? The next section addresses that question.
Diagnostic Approaches to Morgellons Disease
Diagnosis is challenging because no single test confirms Morgellons disease. Healthcare providers typically begin by ruling out known dermatologic, infectious, or systemic conditions that could cause similar symptoms—such as scabies, eczema, neuropathy, or thyroid disorders.
Common steps include:
- Thorough skin examination and history review
- Skin biopsies to analyze lesions and any collected materials
- Microscopic or chemical analysis of fibers (often revealing textile or keratin origin)
- Blood tests to exclude infections, autoimmune issues, or nutritional deficiencies
- Psychiatric evaluation if delusions or obsessive behaviors are prominent
The CDC study emphasized that fibers were not emerging biologically from the skin but resulted from external contamination and chronic excoriation. If symptoms persist despite negative tests, providers may explore underlying psychological factors. Have you considered how these overlapping symptoms could point to different root causes?
Current Approaches to Management and Treatment
There is no proven, standardized treatment for Morgellons disease due to the lack of consensus on its nature. Management focuses on symptom relief, wound care, and addressing any contributing factors.
Common strategies include:
- Topical treatments for itching and skin irritation (e.g., moisturizers, low-potency steroids)
- Wound care to prevent secondary infections
- Medications to reduce sensations of crawling or itching (antihistamines, gabapentin in some cases)
- Psychiatric support, such as cognitive behavioral therapy or antipsychotic medications, particularly when delusional beliefs are central
- Multidisciplinary care involving dermatologists, psychiatrists, and primary providers
In cases where underlying conditions like anxiety or depression are identified, targeted therapy often brings improvement. A supportive, non-confrontational approach helps build trust—patients often feel unheard after multiple consultations. Small studies have explored antibiotics in suspected infectious cases, but evidence remains limited and inconsistent.
Comparing Key Features: Morgellons vs. Related Conditions
| Aspect | Morgellons Disease Reports | Delusional Infestation (Classic) | Known Dermatologic Conditions (e.g., Scabies) |
|---|---|---|---|
| Fiber Perception | Multicolored fibers emerging from skin | Parasites or bugs, no fibers | Actual mites or burrows visible |
| Skin Findings | Self-inflicted erosions, slow-healing sores | Excoriations from scratching | Burrows, papules, intense nocturnal itch |
| Lab Evidence | Fibers usually textile/keratin | No organisms found | Mites/eggs on microscopy |
| Response to Treatment | Variable; psychiatric support often key | Antipsychotics frequently effective | Antiparasitics resolve quickly |
This table illustrates why thorough evaluation is essential—symptoms can overlap significantly.
Safe Next Steps If You Suspect Morgellons Symptoms
If you’re experiencing persistent skin sensations, non-healing sores, or the belief that fibers are involved, start by seeing a dermatologist or primary care provider. Document symptoms carefully, avoid excessive picking to prevent worsening lesions, and be open to multiple perspectives on care.
A compassionate team can help rule out treatable conditions and provide relief for distressing symptoms. Early intervention often improves outcomes, even when the exact cause remains unclear.
This article is for informational purposes only and is not a substitute for professional medical advice. Always consult your healthcare provider for personalized guidance, diagnosis, or treatment.
Living with unexplained skin symptoms can feel isolating, but you’re not alone. Seeking help from trusted professionals is a powerful step toward relief and understanding. If these descriptions resonate, don’t hesitate to discuss them openly with your doctor.






