Have you noticed how conversations about uterine fibroids seem to be happening earlier these days? What used to be considered a concern mainly for women in their 40s is now appearing in younger age groups, sometimes even in the mid-20s. Imagine a 28-year-old woman discovering unexpected pelvic pressure or heavier periods during what should be her most energetic years. The frustration is real—especially when it disrupts work, relationships, or plans for starting a family.

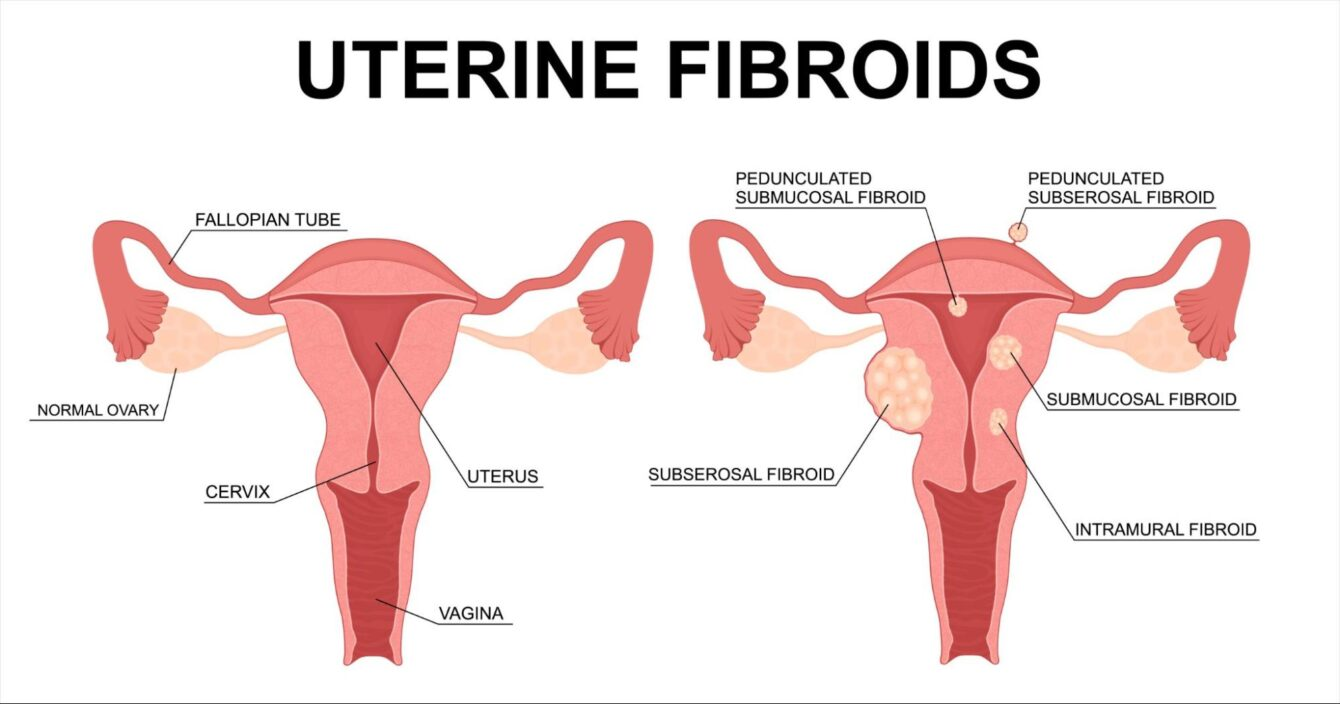
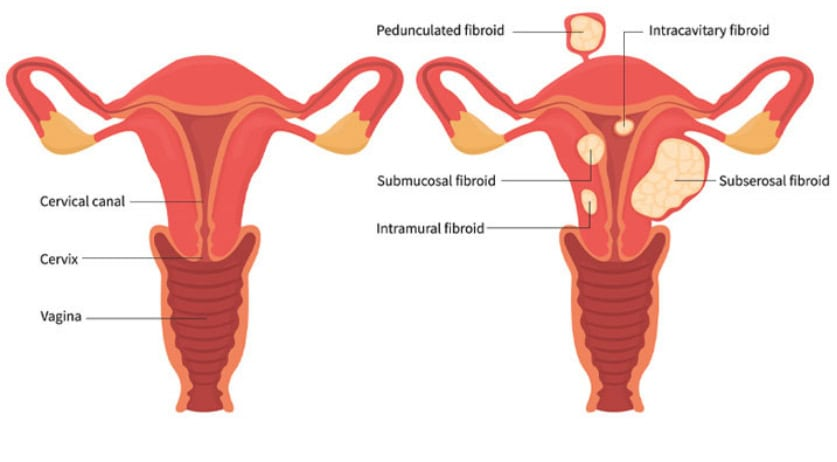
Uterine fibroids, those noncancerous growths in the uterus, affect millions and can cause symptoms like heavy bleeding, pain, and fertility challenges. While they’re extremely common overall (up to 70-80% of women by age 50), recent trends suggest they’re being detected—and sometimes causing issues—at younger ages for more women. Research from global health studies and clinical observations points to several contributing factors. Could modern lifestyles, environmental changes, or other influences be playing a role? Let’s explore the key reasons that experts are discussing, while remembering that fibroids remain under hormonal influence and individual experiences vary widely.
The Growing Awareness of Earlier Onset
Fibroids have always been linked to reproductive years, but data show a shift. Global Burden of Disease studies indicate rising age-standardized incidence in certain regions, with some areas reporting younger onset alongside rapid socioeconomic changes. In the U.S., while overall diagnosis trends have fluctuated, certain groups experience fibroids at notably earlier ages.
What might be driving this? Several interconnected factors appear to contribute. Let’s count down six prominent ones that research highlights.
Reason 6: Earlier Age at Menarche and Prolonged Hormonal Exposure
Many women today start menstruating earlier than previous generations. Early menarche means longer lifetime exposure to estrogen and progesterone—the hormones that fuel fibroid growth.
Studies consistently link earlier puberty onset to increased fibroid risk. In a world where improved nutrition and other factors accelerate development, this extended hormonal window may allow fibroids to begin forming sooner. You might be thinking, “But puberty has always varied”—true, yet population-level shifts add up over time. This sets the stage for even more surprising influences.
Reason 5: Lifestyle Changes and Rising Obesity Rates
Obesity is a well-established risk factor, and rates have climbed steadily among younger adults. Excess body fat can increase estrogen production, creating an environment where fibroids thrive.
Research shows higher BMI correlates with greater risk, possibly through altered hormone metabolism and inflammation. For women in their 20s and 30s facing modern stressors like sedentary jobs or fast-paced eating, this factor often compounds others. But wait—the next reason involves something even more widespread in daily life.
Reason 4: Exposure to Endocrine-Disrupting Chemicals (EDCs)
Modern environments are filled with chemicals that mimic or interfere with hormones—think plastics, personal care products, pesticides, and more. These endocrine disruptors (like phthalates, parabens, BPA, and others) have been associated with reproductive issues, including fibroids.
Animal studies and human epidemiology suggest developmental or ongoing exposure may reprogram cells, increasing susceptibility. Some research links higher EDC levels to earlier or more severe fibroid development. With these ubiquitous in everyday items, many wonder about cumulative effects. Yet this leads to an even more critical point about genetics.
Reason 3: Genetic and Familial Predisposition Amplified in Younger Generations
Family history remains one of the strongest predictors—if your mother or sister had fibroids, your risk rises significantly. Certain genetic variations may make some women more vulnerable.
In younger cohorts, better awareness and earlier screening mean fibroids get detected sooner in those genetically predisposed. Combined with other factors, this can manifest as earlier symptoms. African American women, for example, often face higher rates and earlier onset due to a mix of genetic and environmental influences. But hold on—racial and ethnic disparities reveal even deeper trends.
Reason 2: Racial and Ethnic Disparities Driving Earlier Detection
Black women experience fibroids at higher rates, often at younger ages, with larger tumors and more severe symptoms. Studies show cumulative incidence can exceed 80% in this group by midlife, compared to lower rates in white women.
These disparities may stem from a combination of genetic factors, higher vitamin D deficiency prevalence, and socioeconomic elements affecting access to care. As awareness grows and diagnostic tools improve, more cases are identified early in these populations. This highlights the need for targeted attention, but there’s one more overarching contributor.
Reason 1: Improved Detection and Greater Health Awareness
Perhaps the most significant shift isn’t necessarily more fibroids forming—it’s that we’re finding them earlier. Advances in imaging (like routine ultrasounds), increased gynecologic awareness, and women seeking care sooner for irregular periods mean earlier diagnoses.
Global studies note that in regions with rising healthcare access and health consciousness, incidence appears to climb—likely due to better detection rather than a true explosion in cases. For young women today, this means timely intervention becomes possible, potentially preventing complications. The empowerment that comes from knowledge changes everything.
Real Stories: Young Women Navigating Earlier Fibroid Experiences
Consider Mia, 32, who experienced heavy bleeding during her first pregnancy attempt. Initially dismissing it as stress, an ultrasound revealed multiple fibroids—something her mother had dealt with in her 40s. The early discovery allowed her to explore options before symptoms worsened.
Similarly, Aisha, 29, noticed pelvic pressure during workouts. Her family’s history prompted quicker action, leading to monitoring and lifestyle adjustments. These stories illustrate how earlier awareness empowers proactive steps, though experiences differ widely.
Key Risk Factors at a Glance
| Factor | How It Contributes | Potential Impact on Younger Women |
|---|---|---|
| Early Menarche | Longer estrogen exposure | Starts hormonal influence sooner |
| Obesity | Increased estrogen production | Common in modern lifestyles |
| Endocrine Disruptors | Hormone disruption, possible epigenetic changes | Ubiquitous in daily products |
| Genetics/Family History | Inherited susceptibility | Manifests earlier with other triggers |
| Racial/Ethnic Background | Higher prevalence in some groups | Often earlier onset and severity |
| Improved Detection | More ultrasounds and awareness | Leads to earlier diagnosis |
This overview shows how multiple elements interact—no single cause explains everything.
Steps to Explore Your Own Risk Mindfully
Wondering what you can do? Start with awareness:
- Track your menstrual cycle and note changes
- Maintain a healthy weight through balanced nutrition and movement
- Choose products with fewer chemicals when possible
- Discuss family history with your doctor
- Schedule regular check-ups, especially if symptoms arise
These habits support overall reproductive health without guarantees.
Addressing Common Concerns
You might wonder, “Are fibroids becoming an epidemic?” Evidence suggests better detection plays a major role, not necessarily a massive increase in occurrence. Another question: “Will this affect my fertility?” Many women with fibroids conceive successfully—early monitoring helps.
Always consult a healthcare provider for personalized insights.
Empower Yourself with Knowledge Today
The trend of fibroids appearing in women in their 20s and 30s reminds us how interconnected our bodies are with modern life. From hormonal timelines to environmental influences, understanding these factors offers a path to proactive care.
Key takeaways: earlier hormonal exposure, lifestyle shifts, potential chemical influences, genetics, disparities, and improved detection all contribute to this pattern. Knowledge empowers you to advocate for your health.
Talk to your gynecologist about any concerns—they can guide screening and options. Share this with friends; awareness benefits everyone.
P.S. Fibroids are almost always benign, and many women manage them successfully with the right support.
This article is for informational purposes only and is not a substitute for professional medical advice—readers are encouraged to consult their healthcare provider for personalized guidance.