You pop a pill for pain, infection, or cholesterol without a second thought. Most days, it’s fine. But what if that same medication is quietly stressing your liver? The liver processes almost everything you swallow, turning toxins into harmless waste. When overloaded, it can inflame, scar, or even fail.
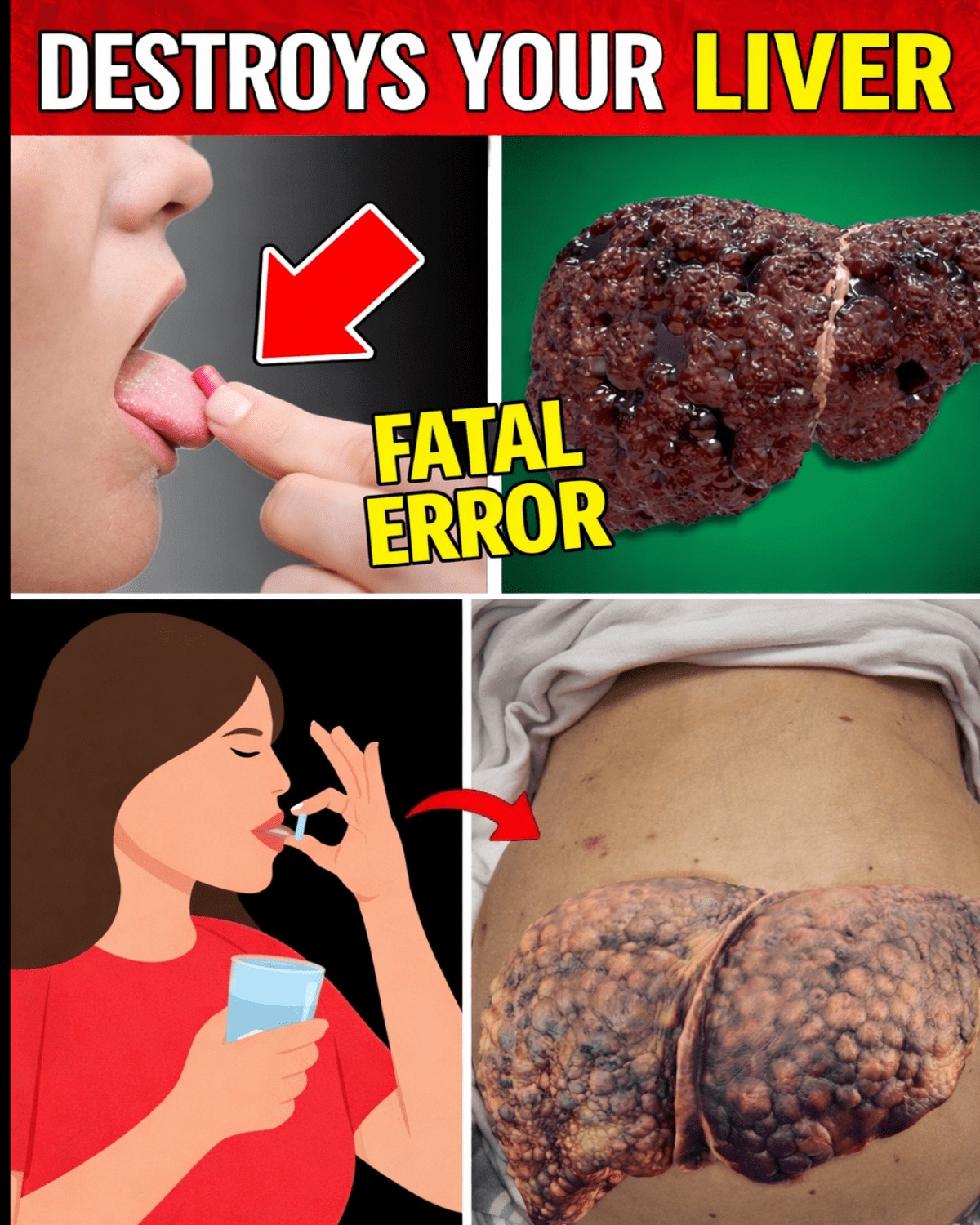
Drug-induced liver injury (DILI) ranks as a leading cause of acute liver failure in the U.S. Many cases stem from common, everyday medications. The scary part? Damage often starts silently, with no obvious pain until things escalate.
Have you noticed unexplained fatigue lately? Or subtle changes in your skin or eyes? These could be clues. Ignoring them risks permanent harm. But awareness changes everything. Let’s explore 10 medications frequently linked to liver stress and the symptoms that signal your liver needs help—before it’s too late.
Why Your Liver Is So Vulnerable to Medications
Your liver filters blood, breaks down drugs, and detoxifies. Some medications overwhelm this system. Acetaminophen causes predictable, dose-dependent damage when overused. Others trigger unpredictable reactions, even at normal doses, due to individual factors like genetics, age, alcohol use, or existing conditions.
Research shows antimicrobials top lists of culprits, followed by pain relievers and supplements. Women, older adults, and those with higher BMI face elevated risks. The good news? Most damage reverses if caught early—by stopping the drug and seeking care.
But first, recognize the red flags.
Early Signs Your Liver May Be Getting Sick
Liver issues often creep in quietly. You might feel “off” without pinpointing why. Common early symptoms include:
- Persistent fatigue or weakness that doesn’t improve with rest
- Loss of appetite, nausea, or mild stomach upset
- Unexplained weight loss
- Dark urine (like tea or cola)
- Pale or clay-colored stools
- Mild abdominal discomfort in the upper right side
- Itchy skin without a rash
As damage progresses, more noticeable signs appear:
- Jaundice (yellowing of skin and eyes)
- Swelling in legs, ankles, or abdomen (edema or ascites)
- Easy bruising or bleeding
- Confusion or brain fog (hepatic encephalopathy in severe cases)
These mimic other issues, so blood tests checking liver enzymes (ALT, AST, ALP, bilirubin) are key. If symptoms emerge after starting a new medication, act fast—contact your doctor.
Ever wonder which common pills pose the biggest threats? Here’s a countdown of 10 medications often associated with liver concerns.
10. Amiodarone (for irregular heartbeats)
This powerful anti-arrhythmic builds up in the body over months or years. It may cause elevated enzymes or, rarely, serious inflammation. Regular monitoring helps catch issues early.
9. Methotrexate (for rheumatoid arthritis or cancer)
Used long-term, it stresses the liver through cumulative effects. Doctors often check enzymes frequently and adjust doses or add protective strategies.
8. Statins (like atorvastatin or simvastatin for cholesterol)
These save lives by lowering heart risk, but rare cases show enzyme spikes or injury. Most resolve by switching statins or lowering doses.
7. Isoniazid (for tuberculosis treatment)
A classic offender, it can cause hepatocellular damage weeks to months in. Risk rises with alcohol use or age.
6. NSAIDs (ibuprofen, naproxen, diclofenac)
Over-the-counter pain relievers seem harmless, but high or prolonged doses strain the liver, especially with other risks like alcohol.
5. Valproic acid (for seizures or bipolar disorder)
It may disrupt liver metabolism, leading to serious issues in some, particularly children or those on multiple meds.
4. Antibiotics like amoxicillin-clavulanate or erythromycin
These rank high in injury reports. Clavulanate combos often cause cholestatic patterns, with jaundice appearing weeks after stopping.
3. Phenytoin or carbamazepine (anti-seizure drugs)
They trigger hypersensitivity reactions affecting the liver, sometimes with rash or fever.
2. Allopurinol (for gout)
Rarely, it sparks severe reactions including liver involvement, often part of broader syndromes.
1. Acetaminophen (Tylenol, paracetamol)
The number-one cause of acute liver failure from meds. Overdoses (even “safe” amounts with alcohol) produce toxic metabolites that destroy cells rapidly.
Research highlights acetaminophen in many emergency cases. Stick to recommended doses—under 4,000 mg daily for most adults, lower if drinking or with liver issues.
How These Medications Compare in Risk and Patterns
Different drugs hit the liver in unique ways. Here’s a quick overview:
| Medication | Common Pattern of Injury | Frequency/Risk Level | Key Monitoring Tip |
|---|---|---|---|
| Acetaminophen | Hepatocellular (dose-dependent) | High in overdose | Never exceed daily limit; avoid alcohol |
| Amoxicillin-clavulanate | Cholestatic/mixed | Common in antibiotics | Watch for jaundice weeks after use |
| NSAIDs (e.g., diclofenac) | Hepatocellular/cholestatic | Low-moderate | Short-term preferred; monitor with chronic use |
| Isoniazid | Hepatocellular | Moderate-high | Baseline + monthly enzyme checks |
| Statins | Hepatocellular (mild) | Rare | Enzymes often normalize without stopping |
| Amiodarone | Mixed | Cumulative over time | Long-term monitoring essential |
This isn’t exhaustive—many others contribute occasionally.
What to Do If You Suspect Liver Trouble
Stop the suspected medication only under medical guidance—sudden stops can harm in some cases. See your doctor promptly for blood work. In severe symptoms like jaundice or confusion, head to emergency care.

Treatment often involves stopping the drug, supportive care, and monitoring. For acetaminophen overdose, N-acetylcysteine acts as an antidote if given early.
Prevention beats reaction every time:
- Share your full medication list (including OTC and supplements) with doctors
- Follow dosing instructions precisely
- Limit alcohol, especially with pain relievers
- Get baseline liver tests for long-term meds
- Report new symptoms immediately
You might think, “This won’t happen to me.” But vigilance protects you.
Take Control Before It’s Too Late
Your liver works tirelessly behind the scenes. Respect it by using medications wisely. Spotting early signs—like nagging fatigue or dark urine—can prevent escalation to serious damage.
Don’t wait for yellow eyes or swelling. Talk to your healthcare provider about your risks, especially if on these meds long-term.
P.S. A simple habit: Review your pill bottles tonight. If anything raises questions, ask your pharmacist or doctor tomorrow.
This article is for informational purposes only and is not a substitute for professional medical advice. Always consult your healthcare provider for personalized guidance before making changes to medications or if you experience symptoms.